Watching your child walk on their toes can be both adorable and concerning. While many toddlers experiment with this gait pattern during development, persistent toe-walking beyond age three often signals underlying issues that deserve attention. As a parent, you’re not alone in searching for effective, gentle solutions that support healthy foot development without causing your little one distress. Orthopedic support booties have emerged as a game-changing intervention, offering targeted correction while allowing children to maintain their natural mobility and playfulness.
These specialized footwear solutions represent more than just shoes—they’re medical devices carefully engineered to retrain muscles, strengthen tendons, and promote proper heel-to-toe walking patterns. Unlike traditional orthotics that can feel bulky or restrictive, modern pediatric booties combine therapeutic benefits with child-friendly designs that encourage consistent wear. Understanding what makes these devices effective, how to select the right features, and when to seek professional guidance can transform your child’s walking journey from uncertain steps to confident strides.
Top 10 Orthopedic Support Booties for Toe-Walkers
Detailed Product Reviews
1. Bunion Corrector for Women Big Toe, Men Too – Ultra-Thin Bunion Sock Separates Big Toes. Soft, Flexible Brace for Inside All Shoes; Dress Shoes, Sneakers & Boots. Protects & Corrects. Small-Left
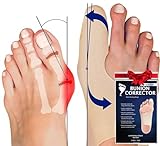
Overview: This ultra-thin bunion corrector offers a discreet solution for mild to moderate hallux valgus. Designed specifically for the left foot in small sizes, this 0.4mm sleeve provides gentle realignment while fitting seamlessly inside virtually any footwear, from dress shoes to boots. Its sock-like construction moves naturally with your foot, making it ideal for all-day wear without bulk or irritation.
What Makes It Stand Out: The remarkable 0.4mm thickness sets this apart from bulky rigid braces. Its flexibility allows natural foot movement while maintaining consistent toe separation. The universal footwear compatibility means you don’t need to change your shoe rotation or compromise daily activities for bunion care. Unlike night splints, this works continuously while you’re active.
Value for Money: At $18.95, this falls in the mid-range for bunion correctors. Compared to custom orthotics ($200+) or surgery (thousands), it’s an affordable conservative treatment. The durable construction withstands daily wear, making it more economical than cheaper alternatives that need frequent replacement. It eliminates need for multiple devices.
Strengths and Weaknesses: Strengths include exceptional thinness, true all-shoe compatibility, and comfortable all-day wear. The flexible design moves naturally with your foot. Weaknesses: limited sizing specificity may not fit all foot shapes, and the gentle correction may be insufficient for severe bunions. Results require consistent, long-term use.
Bottom Line: Ideal for active individuals with mild to moderate left-foot bunions seeking discreet correction. Perfect for professionals who wear dress shoes daily. Not a substitute for medical treatment in advanced cases, but an excellent first-line conservative therapy that delivers comfort without lifestyle disruption.
2. Bunion Corrector for Men Big Toe, Women Too – Ultra-Thin Separator Sock for Mens Bunions. Correction & Pain Relief While You Walk. Splint That Fits in Dress Shoes, Sneakers & Boots. Med-Left

Overview: This medium-sized left-foot bunion corrector delivers targeted relief through an exceptionally thin 0.4mm sleeve design. Engineered for both men and women, it provides discreet toe separation and alignment while maintaining complete footwear compatibility for uninterrupted daily activity. The medical-grade material offers consistent support without compression discomfort.
What Makes It Stand Out: The sock-like flexibility combined with clinical-grade correction distinguishes this from traditional rigid splints. Its ability to function effectively inside narrow dress shoes while providing continuous alignment during walking makes it uniquely practical for professional environments. The medium sizing accommodates a broader range of foot widths than small sizes.
Value for Money: Priced at $18.95, it competes favorably with bulkier braces costing $25-40. The multi-shoe versatility eliminates need for separate orthotic footwear, saving additional expense. For moderate bunion management, it offers better long-term value than disposable spacers or pads. It’s washable and reusable for extended lifespan.
Strengths and Weaknesses: Strengths include superior shoe integration, breathable material, and non-slip design that stays positioned during activity. The gentle correction suits those with sensitivity to rigid devices. Weaknesses: medium sizing may not accommodate wider feet, and the subtle realignment requires months of consistent use for noticeable improvement.
Bottom Line: An excellent choice for left-foot bunion sufferers needing medium sizing who refuse to compromise footwear choices. Best for proactive prevention and mild correction rather than advanced deformity reversal. Delivers exceptional comfort and discretion for daily wearers across diverse activities.
3. BraceAbility Short Walking Boot - Orthopedic Medical Walker Cast for Broken Toe Injuries, Sprained Ankles, Metatarsal Stress, Post-Op Support Left or Right Foot Fracture Shoe Fits Men and Women (L)

Overview: This clinical-grade short walking boot provides protected mobility for serious foot and ankle injuries. Size Large accommodates men’s 10.5-12.5 and women’s 11+, offering ambulatory support for fractures, sprains, and post-operative recovery while maintaining essential immobilization. The bilateral design fits either foot, adding versatility.
What Makes It Stand Out: The rocker bottom sole promotes natural gait mechanics, reducing compensatory injuries. Medical-grade Velcro straps allow precise compression adjustments for swelling fluctuations. The open-toe design accommodates bandaging while the reinforced polymer shell provides institutional-level protection without the institutional aesthetic, making home recovery more comfortable.
Value for Money: At $44.99, it’s competitively priced against medical supply store equivalents ($60-100) and surgical boots. Purchasing often costs less than renting for 4+ weeks. The durable construction supports extended wear throughout recovery, making it a cost-effective alternative to crutches or wheelchairs for ambulatory patients needing protection.
Strengths and Weaknesses: Strengths include proven clinical efficacy, superior adjustability, and bilateral design for either foot. The deluxe foam liner prevents pressure sores during extended wear. Weaknesses: bulky profile limits footwear options, the rigid structure requires adaptation period, and sizing is critical—improper fit compromises therapeutic benefit and comfort.
Bottom Line: Essential for patients requiring protected weight-bearing during recovery. Perfect for post-op bunion surgery, metatarsal fractures, or severe sprains. Consult your physician for proper sizing. A worthwhile investment for safe, independent mobility during healing that outperforms cheaper generic alternatives in comfort and protection.
4. BraceAbility Short Walking Boot - Orthopedic Medical Walker Cast for Broken Toe Injuries, Sprained Ankles, Metatarsal Stress, Post-Op Support Left or Right Foot Fracture Shoe Fits Men and Women (S)
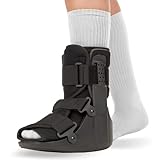
Overview: This orthopedic walking boot in size Small delivers medical-grade immobilization for foot and toe injuries in smaller feet. Designed for both left and right feet, it enables protected ambulation during recovery from fractures, sprains, and post-surgical healing while maintaining therapeutic support and preventing re-injury.
What Makes It Stand Out: The size-specific engineering ensures proper proportional support for smaller foot dimensions, preventing the slippage common in universal-fit boots. The low-profile rocker bottom and adjustable medical Velcro straps provide customized stabilization that adapts to daily swelling variations throughout recovery, ensuring consistent protection.
Value for Money: Priced at $44.99, this small-size boot matches its large counterpart’s value proposition, offering professional-grade protection at consumer pricing. For patients with petite feet, the proper fit eliminates need for costly modifications or compromises in support that generic adjustable boots require, making it economically sound.
Strengths and Weaknesses: Strengths include precise sizing for smaller feet, lightweight polymer construction, and breathable foam liner for extended comfort. The bilateral design adds versatility. Weaknesses: small size range may not fit growing adolescents, the rigid shell demands careful sizing verification, and it’s unsuitable for severe edema beyond initial adjustment capacity.
Bottom Line: Critical for smaller-footed patients requiring reliable immobilization. Ideal for petite women or smaller men recovering from foot trauma. Ensure accurate sizing before purchase. Delivers hospital-quality protection and mobility for home recovery, making it superior to one-size-fits-all alternatives that compromise therapeutic outcomes through poor fit.
5. Bunion Corrector for Women Big Toe &, Men - Ultra-Thin Bunions Sock. Hallux Valgus Splint for Inside All Shoes; Dress Shoes, Sneakers & Boots. Big Toe Protector Sleeve. Med-Right

Overview: This medium-right bunion corrector provides discreet hallux valgus therapy through an ultra-thin 0.4mm sleeve that integrates seamlessly into any footwear. The soft, flexible design delivers continuous toe separation and protection for active users requiring right-foot specific correction during walking, standing, and exercise.
What Makes It Stand Out: The asymmetric design specifically targets right-foot mechanics, while the proprietary 0.4mm material maintains structural integrity despite extreme thinness. Its ability to prevent toe overlap during dynamic activities like running or hiking sets it apart from static night splints that can’t accommodate movement or fit in athletic shoes.
Value for Money: At $18.95, it represents solid mid-market value. The multi-activity versatility eliminates need for sport-specific bunion devices, consolidating costs. Compared to monthly podiatry visits or custom orthotics, it’s an accessible entry point into conservative bunion management with immediate pain relief benefits and long-term preventive value.
Strengths and Weaknesses: Strengths include targeted right-foot design, exceptional breathability, and washability for hygiene. The flexible reinforcement prevents material fatigue. Weaknesses: medium sizing lacks half-size options, the subtle correction requires patience, and it may migrate during high-impact activities without proper sock anchoring or adjustment.
Bottom Line: Perfect for right-foot bunion sufferers seeking unobtrusive daily correction. Excellent for athletes and professionals who need consistent support across various shoe types. Most effective when combined with proper footwear choices. A practical, affordable solution for managing progression and discomfort without activity limitation.
6. BraceAbility Short Walking Boot - Orthopedic Medical Walker Cast for Broken Toe Injuries, Sprained Ankles, Metatarsal Stress, Post-Op Support Left or Right Foot Fracture Shoe Fits Men and Women (XS)

Overview: The BraceAbility Short Walking Boot delivers clinical-grade protection for foot and ankle injuries. Designed to treat broken toes, metatarsal fractures, sprains, and post-operative conditions, this medical walker provides immobilization while maintaining mobility. The universal design fits either foot, making it versatile for various recovery scenarios.
What Makes It Stand Out: This boot’s clinical validation sets it apart from generic alternatives. The deluxe foam liner ensures comfort during extended wear, while the wide toe bed and open-toe design accommodate swelling and bandaging. The low-profile rocker bottom promotes a natural gait pattern, and the rigid polymer plastic shell offers robust protection on both sides of the foot and ankle.
Value for Money: At $44.99, this boot sits in the mid-range price category. The investment is justified by its medical-grade construction and proven therapeutic benefits. While budget options exist, they lack the clinical backing and premium features like the rocker bottom and deluxe liner that facilitate proper healing and comfort.
Strengths and Weaknesses: Strengths include clinically proven protection, superior comfort from the foam liner, adjustable Velcro straps for customized fit, and the rocker bottom that enables natural walking. The universal left/right design adds convenience. Weaknesses include potential sizing challenges—users must carefully consult the chart—and the bulkier profile compared to post-op shoes. Some may find the price steep versus basic models.
Bottom Line: The BraceAbility boot excels for moderate to severe injuries requiring reliable immobilization. Its clinical pedigree and thoughtful design make it worth the premium for serious recovery.
7. Short Walking Boot Fracture Boot Air Walker Boot for Orthopaedic Boot for Sprained Ankle, Walker Brace for Broken Foot Achilles Tendon Injury (Medium)

Overview: This Short Walking Boot features an innovative inflatable air bladder system that adapts to your recovery journey. Suitable for sprained ankles, broken feet, and Achilles tendon injuries, it provides adjustable compression and support throughout healing stages. The medium size targets average adult dimensions.
What Makes It Stand Out: The adjustable inflatable design is the star feature, allowing users to modify internal pressure as swelling fluctuates. Early-stage deflation prevents painful pressure, while later inflation ensures snug support. Strong, ergonomic materials create a protective frame, and the lightweight construction reduces fatigue during mobility.
Value for Money: Priced at $36.99, this boot offers excellent value for air bladder technology. Similar medical-grade air walkers often cost $50+, making this an accessible option without sacrificing core functionality. The ability to customize fit across recovery phases adds significant long-term value.
Strengths and Weaknesses: Strengths include the adaptable inflation system, quality supportive materials, comfortable sponge lining, lightweight build, and easy Velcro adjustments. The ergonomic design fits natural leg contours. Weaknesses involve potential durability concerns with the inflation mechanism over months of use, and sizing may run small for some users. The plastic components lack the premium feel of higher-end brands.
Bottom Line: Ideal for injuries with significant swelling fluctuations, this air walker delivers customizable support at a competitive price. It’s a smart choice for dynamic recovery needs.
8. Vive Offloading Post-Op Shoe - Forefront Wedge Boot for Broken Toe Injury - Non Weight Bearing Medical Recovery for Foot Surgery, Hammer Toes, Bunion, Feet Walking Orthopedic (Medium)

Overview: The Vive Offloading Post-Op Shoe specializes in protecting the forefoot and toes during recovery. Engineered for broken toes, bunion surgery, hammertoe correction, and diabetic foot ulcers, this wedge-design shoe shifts weight to the heel, minimizing pressure on vulnerable areas.
What Makes It Stand Out: The dorsiflexion angled wedge is the key innovation, actively offloading the forefoot to promote healing. A wide, square toe box acts as a protective bumper, while dense foam padding cushions sensitive areas. The design accommodates bulky bandages through adjustable straps and extender tabs.
Value for Money: At $29.99, this specialized shoe offers strong value for its targeted function. While not a universal boot, its specific design for forefoot offloading justifies the cost compared to using a standard walking boot that doesn’t address pressure redistribution.
Strengths and Weaknesses: Strengths include effective pressure offloading, lightweight nonskid rubber base, excellent toe protection, and easy adjustability for swelling. The neutral base fits either foot. Weaknesses include limited applicability—it’s unsuitable for ankle or midfoot injuries. The wedge design feels unnatural initially, and sizing runs small. It provides less overall stability than full boots.
Bottom Line: For forefoot-specific injuries requiring pressure relief, the Vive offloading shoe is an excellent, affordable solution. Choose this when toe protection is paramount.
9. Post Op Shoe Broken Toe Open Walking Shoe Lightweight Surgical Foot Protection Cast Boot Adjustable Straps for Ankle Injures Support Bunion Hammertoe Post Surgery Brace Foot Fracture Orthopedic Shoe

Overview: This budget-friendly Post Op Shoe provides basic protection for minor foot and ankle injuries. Constructed from canvas with a non-slip synthetic sole, it offers a lightweight, breathable alternative to rigid boots for conditions like toe fractures, bunions, and plantar fasciitis recovery.
What Makes It Stand Out: The open-toe and heel design maximizes breathability, preventing overheating during extended wear. The curved sole reduces ankle movement while promoting a more natural step. Adjustable elastic bands provide easy tightening, and the wide toe box eliminates binding for swollen feet.
Value for Money: At just $18.99, this is the most economical option for post-operative protection. While lacking advanced features, it delivers essential functionality at a fraction of medical supply store prices. It’s ideal for short-term use or minor injuries where full immobilization isn’t required.
Strengths and Weaknesses: Strengths include exceptional affordability, lightweight breathability, easy adjustability, and versatile sizing. The canvas material is comfortable against skin. Weaknesses include limited support—the canvas construction can’t match rigid plastic protection. Durability concerns arise with heavy use, and it’s inappropriate for severe fractures or significant instability. The aesthetic is distinctly medical and basic.
Bottom Line: This shoe serves well for minor injuries, short-term recovery, or budget-conscious users. For serious conditions, invest in a more robust boot.
10. Jewlri Walking Boot, Short Air Walker Fracture Boot Support for Broken Foot Sprained Ankle Fracture Recovery fits Left or Right Foot Black Medium

Overview: The Jewlri Walking Boot offers solid mid-range support for fracture recovery. This short air walker features a rigid plastic frame and rocker sole design, providing stabilization for broken feet, sprained ankles, and post-operative healing. The unisex medium size fits either foot interchangeably.
What Makes It Stand Out: The whole-shaped rigid plastic shell uses advanced molding technology for enhanced stability without excessive weight. The rocker bottom sole provides arch support and promotes natural gait mechanics. A removable, washable liner maintains hygiene during extended recovery periods.
Value for Money: At $39.83, this boot strikes an excellent balance between quality and affordability. It undercuts premium brands while delivering essential features like the rocker sole and rigid protection. The washable liner adds long-term value that disposable liners lack.
Strengths and Weaknesses: Strengths include sturdy construction, comfortable thick insole, effective rocker bottom for natural walking, easy adjustability, and the convenience of a washable liner. The unisex design simplifies ordering. Weaknesses include limited brand recognition compared to established medical suppliers, potential sizing inconsistencies, and basic strap hardware. The air bladder system is less sophisticated than premium models.
Bottom Line: A reliable, well-priced choice for typical fracture recovery needs. It provides core functionality without unnecessary frills, making it practical for most users seeking dependable support.
Understanding Toe-Walking in Children
What is Toe-Walking?
Toe-walking refers to a gait pattern where a child walks on the balls of their feet without their heels touching the ground. While occasional toe-walking is normal during early walking development, persistent toe-walking becomes clinically significant when it continues beyond 18-24 months of age. This pattern can be either unilateral (affecting one foot) or bilateral (affecting both feet), with bilateral presentation being more common in idiopathic cases.
The mechanics of toe-walking place abnormal stress on developing foot structures. The plantar fascia remains shortened, calf muscles (gastrocnemius and soleus) develop increased tone, and the Achilles tendon may lose flexibility over time. This creates a cyclical problem: the more a child toe-walks, the tighter these structures become, making heel-to-toe walking increasingly difficult without intervention.
When Toe-Walking Becomes a Concern
Most children achieve a mature heel-to-toe gait pattern by 18 months, with consistent heel strike by age two. If your child continues to toe-walk more than 50% of the time after their third birthday, pediatric specialists recommend evaluation. Red flags that warrant immediate consultation include:
- Inability to stand with heels flat on the ground when stationary
- Tightness or pain in calf muscles
- Frequent falls or balance issues
- Delayed gross motor milestones
- Toe-walking that interferes with participation in age-appropriate activities
- Family history of neurological conditions
Early intervention typically yields better outcomes, as younger children’s musculoskeletal systems are more pliable and responsive to corrective measures. The window between ages two and five represents an optimal treatment period where conservative interventions like orthopedic booties can be highly effective.
Common Causes and Diagnosis
Idiopathic toe-walking, accounting for approximately 5-12% of persistent cases, occurs without identifiable neurological or orthopedic cause. However, toe-walking can also signal underlying conditions requiring specific treatment approaches. Common etiologies include:
- Neurological conditions: Cerebral palsy, muscular dystrophy, or tethered spinal cord
- Developmental disorders: Autism spectrum disorder (present in 20-30% of children with ASD)
- Anatomical limitations: Congenital short Achilles tendon or structural foot abnormalities
- Sensory processing issues: Seeking proprioceptive input or avoiding certain textures
A comprehensive diagnostic workup typically involves pediatric orthopedic or neurology specialists, physical therapists, and sometimes developmental pediatricians. Assessment includes range of motion testing, neurological examination, gait analysis, and evaluation of family history. This thorough approach ensures that support booties are prescribed appropriately and address the root cause rather than just the symptom.
The Role of Orthopedic Support Booties
How Support Booties Help Correct Toe-Walking
Orthopedic support booties function through a multi-modal approach to gait correction. Unlike rigid braces that forcibly hold the foot in position, therapeutic booties provide sensory feedback and gentle mechanical guidance that encourages natural pattern retraining. The design typically features a firm heel counter that makes toe-walking biomechanically less efficient while a flexible forefoot allows normal push-off during proper gait.
These devices work by creating a “sensory reminder”—when a child attempts to rise onto toes, the bootie’s construction provides subtle resistance, prompting them to engage heel contact instead. Over weeks to months of consistent wear, this repetitive correction helps establish new neural pathways, essentially retraining the brain’s motor planning for walking. Simultaneously, the booties maintain the foot in a slightly dorsiflexed position during rest periods, providing passive stretching of tight posterior chain structures.
The Science Behind Orthopedic Intervention
The effectiveness of support booties rests on principles of neuroplasticity and tissue adaptation. Children’s developing nervous systems exhibit remarkable ability to reorganize neural connections in response to consistent sensory input and movement patterns. By providing tactile and proprioceptive feedback at critical moments in the gait cycle, booties help establish corrected motor engrams—pre-programmed movement patterns stored in the brain.
From a biomechanical perspective, these devices address the equinus deformity (limited ankle dorsiflexion) characteristic of persistent toe-walking. The controlled positioning allows for gradual, safe lengthening of the triceps surae muscle complex without the risks associated with aggressive stretching or surgical intervention. Research demonstrates that consistent orthotic intervention combined with physical therapy can improve ankle dorsiflexion by 10-15 degrees over a 6-12 month period in children with idiopathic toe-walking.
Differences Between Booties and Other Orthotic Devices
Support booties occupy a unique space in the orthotic continuum, distinguishing themselves from both traditional ankle-foot orthoses (AFOs) and simple shoe inserts. Unlike AFOs, which extend up the calf and provide rigid control, booties offer more freedom of movement while still delivering targeted correction. This makes them ideal for children with mild to moderate toe-walking who don’t require extensive mechanical support.
Compared to over-the-counter orthotic insoles, booties provide comprehensive foot control rather than just arch support. The external construction influences foot position throughout the entire gait cycle, not just during weight-bearing. Additionally, booties eliminate the “toe-walking in the orthotic” phenomenon where children simply rise onto toes despite wearing inserts inside conventional shoes.
Key Features to Look for in Pediatric Orthopedic Booties
Anatomical Design and Foot Shape
The foundation of effective support booties lies in their anatomical accuracy. Look for designs that mirror the natural shape of a child’s foot, including a wide toe box that allows toe splay and proper weight distribution. The heel cup should be deep and contoured to cradle the calcaneus securely, preventing slippage that could compromise correction.
Pediatric foot anatomy differs significantly from adult feet. Children have proportionally wider forefeet, softer cartilage, and rapidly changing bone structure. Quality booties accommodate these differences with flexible but supportive materials that don’t compress developing bones. The last (foot model used in design) should reflect pediatric proportions, not simply scaled-down adult dimensions.
Material Quality and Breathability
Children’s feet perspire significantly more than adult feet—approximately twice as much per square centimeter. This physiological reality demands materials that manage moisture effectively to prevent skin breakdown, odor, and discomfort that could lead to non-compliance. Premium options utilize medical-grade, hypoallergenic leather or advanced synthetic microfibers with built-in antimicrobial properties.
The interior lining should be seamless or have flat seams to prevent friction points, particularly around the heel and ankle where pressure is greatest. Some designs incorporate moisture-wicking linings similar to athletic performance fabrics, while others use natural materials like merino wool blends that regulate temperature and resist bacterial growth. Avoid booties with plastic or vinyl components that trap heat and moisture against delicate skin.
Sole Construction and Flexibility
The outsole represents a critical engineering element in support booties. It must provide enough rigidity at the heel to discourage toe-walking while maintaining forefoot flexibility for natural propulsion. Look for soles with a “stiffness gradient”—firmer at the heel, progressively more flexible toward the toes.
Rubber compound quality affects both durability and grip. Medical-grade rubber should provide secure traction on various surfaces without being sticky or leaving marks. The heel height differential (drop) typically ranges from 4-8mm in therapeutic booties, subtly encouraging heel strike without creating an unnatural feeling. Some advanced designs incorporate rocker-bottom elements that facilitate smooth heel-to-toe transition during gait.
Adjustability and Growth Accommodation
Children’s feet grow rapidly—typically one full size every 3-4 months during early childhood. Quality support booties must accommodate this growth without compromising therapeutic effectiveness. Look for designs with multi-point adjustability: removable insoles that can be modified, adjustable straps or laces, and expandable upper constructions.
Some premium options feature “growth zones”—sections of elasticized material or additional eyelets that allow the bootie to expand horizontally and vertically. The best designs provide 6-9 months of usable life despite growth, representing both economic value and consistent therapeutic intervention. Avoid booties sized by age ranges alone; precise sizing charts based on foot measurements are essential for proper fit.
Closure Systems for Secure Fit
The closure mechanism directly impacts both effectiveness and child cooperation. Traditional laces offer the most customizable fit but can be challenging for young children to manage independently. Hook-and-loop (Velcro) closures provide easy adjustability and are ideal for children with fine motor difficulties, though they may lose grip strength over time.
Buckle systems, particularly those with micro-adjustment capabilities, combine security with ease of use. Some innovative designs incorporate BOA-style dial closures, allowing precise tension adjustment with one hand. Regardless of style, closures should be positioned to avoid pressure points on bony prominences and should be easily operable by parents while being child-resistant enough to prevent removal.
Weight Considerations for Active Kids
Every additional ounce on a child’s foot increases metabolic cost and can discourage consistent wear. Modern orthopedic booties leverage lightweight materials like carbon fiber reinforced polymers and EVA foam to minimize weight while maintaining structural integrity. Aim for booties that weigh no more than 6-8 ounces per shoe for toddlers and 8-10 ounces for school-age children.
The weight distribution matters as much as total weight. Heavier elements should be positioned closer to the foot’s natural center of mass to reduce the pendulum effect during swing phase. Some manufacturers achieve this through strategic material placement, using denser compounds only where structural support is absolutely necessary.
Getting the Right Fit: A Professional Approach
Importance of Professional Measurement
While online sizing guides provide a starting point, professional fitting by a pediatric orthotist or physical therapist ensures optimal therapeutic outcomes. These specialists use brannock devices modified for pediatric feet, measure arch length in addition to overall length, and assess foot width at multiple points. They also evaluate dynamic foot function—how the foot behaves during weight-bearing and gait.
Professional fitting sessions should include assessment of ankle range of motion while the child wears the booties, verification of heel seating in the cup, and observation of walking patterns. Many orthotic clinics use pressure mapping technology to identify areas of excessive force that could lead to skin issues or discomfort. This data-driven approach fine-tunes fit in ways impossible through visual assessment alone.
At-Home Fitting Tips
If professional fitting isn’t immediately accessible, several at-home techniques improve fit accuracy. Measure both feet at the end of the day when they’re largest, and always fit to the larger foot. Have your child stand on a piece of paper while you trace the foot, then measure length from heel to longest toe and width at the ball of the foot.
When trying booties, check for a thumb’s width of space between the longest toe and the bootie end. The heel should sit snugly in the cup without lifting during toe raises. Have your child walk and observe whether the heel stays seated and if any redness appears after five minutes of wear. Remove the insole and have your child stand on it—their foot should fit within the borders without hanging over edges.
Signs of Proper vs. Improper Fit
Properly fitted booties feel comfortable enough that children forget they’re wearing therapeutic devices. Positive indicators include: ability to run and climb normally, no complaints of pain after the initial break-in period, even wear patterns on the soles, and gradual improvement in heel-to-toe gait. The booties should stay in place without requiring constant readjustment.
Warning signs of poor fit demand immediate attention: persistent red marks lasting more than 20 minutes after removal, blisters or callus formation, complaints of numbness or tingling, excessive heel slippage, or the child consistently trying to remove the booties. If your child develops a limp or altered gait pattern different from their baseline toe-walking, the booties may be overly restrictive or improperly aligned.
Age-Specific Considerations
Infants and Toddlers (12-24 months)
At this developmental stage, the primary goal is encouraging natural movement patterns without restricting exploration. Booties for this age group should be exceptionally lightweight and flexible, focusing more on sensory input than rigid correction. The design should accommodate the fat pad in the infant foot, which provides natural cushioning but disappears by age two.
Look for booties with minimal heel elevation and maximum ground feel. The closure system must be secure enough that curious toddlers can’t easily remove them, yet comfortable enough for all-day wear during active play. Since children this age can’t verbalize discomfort, visual inspection of skin and behavior monitoring become critical compliance indicators.
Preschool Age (2-4 years)
This age group represents the sweet spot for orthotic intervention, as children are developmentally ready to respond to corrective feedback but haven’t developed fixed contractures. Booties for preschoolers can incorporate more structured elements while still allowing dynamic movement. The design should support independence—children should be able to put on and remove booties with minimal assistance.
Aesthetic considerations become increasingly important; preschoolers begin noticing differences between their shoes and peers’. Many manufacturers offer colorful designs or customizable elements that make therapeutic booties feel special rather than medical. Durability becomes paramount as these children engage in more vigorous play, requiring reinforced toe caps and scuff-resistant materials.
School-Age Children (5+ years)
Older children present unique challenges: they’re more self-conscious about appearance, engage in diverse physical activities, and can articulate specific discomforts. Support booties for this group must balance therapeutic effectiveness with social acceptability. Many designs mimic athletic shoes or trendy boots, camouflaging their medical purpose.
These booties often incorporate more robust correction mechanisms since untreated toe-walking has become more entrenched. However, they must also accommodate school activities—from sitting cross-legged during circle time to running during recess. Some designs feature interchangeable components that adjust correction level based on activity, allowing more freedom during physical education while maintaining support during classroom time.
Working with Healthcare Professionals
When to Consult a Pediatric Podiatrist
While your pediatrician provides excellent general guidance, pediatric podiatrists specialize in foot and ankle development. Consultation becomes essential if toe-walking persists beyond age three, is associated with pain, or shows asymmetrical patterns. Podiatrists can differentiate between structural, neurological, and idiopathic causes, ensuring bootie prescription matches the underlying etiology.
These specialists perform comprehensive gait analysis, often using video recording and computer software to quantify parameters like heel strike angle, stride length, and ankle kinematics. They can also identify subtle foot deformities like metatarsus adductus or calcaneovalgus that complicate toe-walking and require specific bootie modifications. Many podiatrists work directly with orthotists to custom-design devices when off-the-shelf options prove insufficient.
The Role of Physical Therapy
Orthopedic booties work synergistically with physical therapy, not as standalone solutions. A pediatric physical therapist develops targeted exercises that address muscle imbalances, improve ankle dorsiflexion range, and strengthen antagonist muscles. They teach parents stretching protocols—like sustained calf stretches with knee extended and flexed—that complement bootie wear.
Therapists also provide activity modifications that encourage heel contact, such as walking backward, heel-walking practice, and sensory activities that desensitize the heel for weight-bearing. Many incorporate balance training and core strengthening, recognizing that toe-walking often correlates with proximal weakness or postural control issues. Regular therapy sessions allow for bootie adjustment as the child progresses.
Creating a Comprehensive Treatment Plan
Effective toe-walking correction requires more than just purchasing booties—it demands a coordinated plan involving parents, therapists, physicians, and educators. The plan should specify daily wear schedules (typically 6-8 hours during weight-bearing activities), break-in periods, and criteria for progression or modification. Document baseline measurements like ankle dorsiflexion range and walking speed to track improvement objectively.
Include school personnel in the plan, providing teachers with information about the booties’ purpose and any activity restrictions. Some children benefit from a “bootie journal” where parents and teachers note compliance, comfort issues, and observed gait improvements. This data helps clinicians make informed decisions about weaning schedules and long-term prognosis.
Daily Use and Care Guidelines
Breaking In Period
Never expect a child to wear new orthopedic booties for full prescribed duration immediately. A gradual break-in period prevents skin breakdown and psychological resistance. Start with 30-60 minutes of wear during pleasant activities like playtime or television watching. Increase duration by 30 minutes daily, monitoring for red flags.
During this period, inspect feet every time booties are removed, checking for pressure points or irritation. Some children benefit from wearing thin, seamless socks initially, even if booties are designed for barefoot wear. Expect some initial complaints about the “weird” feeling of heel contact—this is normal and typically resolves within one to two weeks as neuromotor patterns begin adjusting.
Recommended Wear Time
Optimal wear time varies by diagnosis and severity. For idiopathic toe-walkers, clinicians typically recommend wearing booties during all weight-bearing activities except sleeping and water activities. This usually translates to 6-10 hours daily. Some protocols suggest full-time wear for the first 3-6 months, then gradual reduction as gait normalizes.
Consistency matters more than total hours. Wearing booties for shorter periods daily proves more effective than sporadic full-day use. Many families find success with a schedule that includes booties during school hours and active playtime at home, allowing barefoot or regular shoes during quiet evening activities. This balance maintains therapeutic benefit while preventing burnout.
Cleaning and Maintenance
Proper care extends bootie lifespan and prevents hygiene issues. Most quality booties feature removable insoles that can be hand-washed with mild soap and air-dried. The exterior requires regular wiping with damp cloths; some leather models benefit from occasional conditioning with pediatric-safe leather balm. Always air dry booties away from direct heat, which can warp structural components.
Inspect booties weekly for wear patterns. Excessive wear on the toe area may indicate persistent toe-walking despite intervention, while uneven heel wear suggests alignment issues requiring adjustment. Check closure systems for proper function—Velcro that no longer grips or stretched elastic compromises fit and effectiveness. Most booties require replacement every 6-12 months due to growth and material fatigue.
Monitoring Progress
Systematic tracking transforms subjective observations into actionable data. Use smartphone video to record your child walking monthly from multiple angles—front, back, and side. Note the percentage of steps showing heel contact, stride symmetry, and any complaints of pain or fatigue. Many parents create simple rating scales for ease of morning donning and end-of-day comfort.
Schedule regular follow-ups with your prescribing clinician every 8-12 weeks during active treatment. They’ll reassess ankle range of motion, gait parameters, and bootie fit. Objective improvement metrics include increased passive ankle dorsiflexion beyond neutral, spontaneous heel-to-toe steps without reminders, and reduced calf muscle tightness. Celebrate small victories—each new skill mastered represents neural rewiring and tissue adaptation.
Insurance and Cost Considerations
Understanding Coverage Options
Orthopedic support booties qualify as durable medical equipment (DME) under most insurance plans when prescribed by a physician for diagnosed conditions. However, coverage varies significantly between policies. Many insurers require documentation of failed conservative treatment attempts, physical therapy participation, and evidence that toe-walking impacts functional activities.
Pre-authorization is often necessary, involving detailed letters of medical necessity from pediatricians or specialists. Some policies cover custom-molded booties but not off-the-shelf options, while others reverse this criteria. Contact your insurance provider early in the process, requesting specific DME coverage details, in-network orthotist requirements, and documentation needed for reimbursement.
Budget-Friendly Strategies
If insurance coverage proves limited, several strategies reduce out-of-pocket costs. Some orthotic clinics offer payment plans or sliding-scale fees based on family income. Manufacturer refurbished programs provide gently used booties at significant discounts, professionally sanitized and reconditioned. Consider purchasing two pairs simultaneously—many suppliers offer discounts on second pairs, and having backup booties prevents treatment gaps when primary pair requires repair.
Community resources may provide assistance. Children’s hospitals often maintain equipment loan programs, and some charitable organizations specifically fund orthopedic devices for families in need. While cost matters, avoid compromising on quality—poorly constructed booties can cause more harm than good, potentially leading to costly complications requiring surgical intervention.
Potential Challenges and Solutions
Child Resistance and Comfort Issues
Even well-designed booties can face resistance from strong-willed children. Frame booties positively—call them “superhero shoes,” “jumping boots,” or another empowering term. Allow children to choose between approved colors or patterns when possible. Implement reward systems for compliant wear, focusing on immediate small rewards rather than distant large ones.
If discomfort persists beyond the break-in period, investigate thoroughly. Sometimes the issue isn’t physical but psychological—a reaction to feeling different from peers. In these cases, working with a child psychologist or occupational therapist familiar with sensory processing can help. For genuine physical discomfort, consult your orthotist about modifications like pressure-relief padding or strap repositioning.
Skin Irritation and Pressure Points
Despite best efforts, pressure-related skin issues occasionally occur. Prevent problems by ensuring booties are completely dry before wear and using moisture-wicking socks if permitted. Apply petroleum jelly or specialized friction-reducing balms to known pressure points proactively. Check feet immediately after removing booties, looking for areas of persistent redness.
If blisters develop, discontinue wear until healed, then reassess fit. Sometimes simple adjustments like adding moleskin padding to problem areas or slightly loosening specific straps resolve issues. Persistent pressure points may indicate the booties are too small, structurally inadequate for your child’s foot shape, or that your child needs custom modifications. Never ignore ongoing skin issues—they can lead to breakdown and infection.
Transitioning Between Shoe Types
The ultimate goal is normalized gait without orthotic dependence. Transition planning should begin once your child demonstrates consistent heel-to-toe walking in booties for several consecutive weeks. Start with short periods in regular shoes during low-impact activities, gradually increasing duration as strength and pattern retention improve.
Some clinicians recommend “weaning booties” with reduced support features as an intermediate step. Others suggest continuing booties for high-impact activities like running while allowing regular shoes for classroom time. Monitor for regression closely during transitions—any return of toe-walking exceeding 25% of steps warrants returning to full-time bootie wear. Successful weaning typically occurs over 2-4 months, not abruptly.
Frequently Asked Questions
How long will my child need to wear orthopedic support booties?
Most children require 6-12 months of consistent wear to establish lasting gait changes, though this varies significantly based on age, severity, and underlying cause. Younger children with idiopathic toe-walking often graduate sooner, while those with neurological conditions may need longer-term support. Your child’s care team will establish specific criteria for weaning based on measurable improvements.
Can my child wear regular socks with orthopedic booties?
Most booties are designed for direct skin contact to maximize sensory feedback and prevent slippage. However, thin, seamless socks made from moisture-wicking materials are acceptable if they don’t compromise fit. Avoid thick or cushioned socks that alter the therapeutic positioning. Always check with your prescribing clinician, as some designs specifically prohibit socks.
Will wearing booties weaken my child’s foot muscles?
Properly designed booties don’t cause muscle weakness—they facilitate proper muscle activation patterns. By positioning the foot correctly, booties actually allow intrinsic foot muscles and anterior compartment muscles to engage more effectively. Many children show improved foot strength after consistent wear because they’re using muscles previously underutilized during toe-walking.
How do I convince my strong-willed toddler to keep booties on?
Success often depends on making booties non-negotiable while creating positive associations. Establish a consistent routine where booties go on immediately upon dressing, before favorite activities. Use distraction during initial donning and praise compliance enthusiastically. Avoid power struggles by remaining calm and matter-of-fact. Some parents find success with social stories or videos showing other children wearing similar devices.
Are there activities my child should avoid while wearing booties?
Most booties accommodate normal childhood activities, but swimming and prolonged water play require removal. Some high-impact sports may necessitate sport-specific orthotics instead. Your child can typically climb, run, and ride bikes safely. Always verify activity restrictions with your bootie manufacturer and clinician, as design variations affect suitability.
What if my child’s feet grow quickly during treatment?
Rapid growth is expected and actually indicates healthy development. Most quality booties accommodate 1-1.5 shoe sizes of growth through adjustable features. Schedule fit checks every 6-8 weeks, and don’t delay ordering larger sizes—wearing too-small booties can cause harm. Some manufacturers offer growth guarantees or discounted replacement programs.
Can toe-walking correct itself without intervention?
Approximately 5-12% of idiopathic toe-walkers spontaneously normalize by age five. However, waiting to see if this occurs risks developing fixed contractures that require more invasive treatment. Given the excellent outcomes with early conservative intervention, most specialists recommend starting booties by age three rather than adopting a watchful waiting approach.
How do I clean booties if they get smelly?
Odor indicates bacterial growth from trapped moisture. Remove insoles daily for airing and wash them weekly with antibacterial soap. Wipe bootie interiors with diluted white vinegar or specialized orthotic cleaning sprays. Ensure complete drying before wear—using a shoe dryer on cool setting helps. Rotating between two pairs allows complete drying between uses and significantly reduces odor.
Will my child need physical therapy in addition to booties?
Most treatment protocols combine booties with physical therapy for optimal results. Therapy addresses underlying muscle tightness, weakness, and motor planning issues that booties alone can’t resolve. The combination approach typically yields faster, more sustainable improvements than either intervention alone. Your child’s specific needs determine therapy frequency and duration.
How can I tell if the booties are actually working?
Track objective metrics: measure ankle dorsiflexion range monthly, video gait analysis, and document the percentage of steps with heel contact. Subjective improvements include reduced toe-walking when barefoot, decreased calf tightness, and spontaneous comments about walking feeling “easier.” Most families notice initial changes within 4-6 weeks, with significant improvement by 3-4 months of consistent use.